Introduction to Your COBRA Files
Now that you have your COBRA files up and running, sending new hires and terminations to your COBRA administrator, it is important to know how the COBRA files will work.
Terms and Definitions
- DOL - Dept of Labor
- NPM – New Plan Member
- QB - Qualified Beneficiary – this can be the employee or dependent
- QE - Qualifying Event
- COBRA Eligible
COBRA (Consolidated Omnibus Budget Reconciliation Act)
COBRA contains provisions giving certain former employees, retirees, spouses, former spouses, and dependent children the right to temporary continuation of health coverage at group rates. Must provide covered employees and their families with specific notices explaining their COBRA rights.
Today we support two notices that translate into the file and sent to your COBRA administrator:
- New Hire/DOL/NPM file generates the Initial Rights Notice
- The QE/Term File generates the Election Notice
New Hire – The NH (NPM or DOL) file will send employees who have just been added to your system. This may be tricky during implementation, as when you first start with Core HR, every employee is new to the system. Trust that the EDI Specialist building your file will sort this out during the file implementation and make sure that only truly new employees will be sent on the file when it moves to production. This however, can be more challenging, during your renewal. The system will only send an employee that has been processed and elected benefits. That is, when you have added an employee into the system and awarded them COBRA eligible benefits (whether the employee uses their portal to make elections or you enter the elections from the administrative portal), this will push the employee’s record to the COBRA log.
Qualifying Beneficiary – Usually titled “QB” or “QE” (Qualifying Event) in the exports. Depending on the type of event, either the employee or the dependent becomes the QB. In both cases either the employee and their dependents or a Dependent have had their benefits terminated. As per the new hire file, the employee must have elected COBRA eligible benefits.
An employee must be terminated correctly and have a termination reason assigned in order to feed correctly over on the file.
A dependent only termination must have their benefits expired correctly and have a COBRA eligible event assigned in order to be included in the file.
COBRA Eligible Benefits:
- Medical
- Dental
- Vision
- Healthcare FSA
*Some states require that Basic Life and Voluntary Life also be offered.
COBRA Events:
- Termination
- Reduction in hours of employment of the covered employee;
- Death of the covered employee
- Covered employee's becoming entitled to Medicare
- Divorce or Legal separation
- A child's loss of dependent status under the plan
At this time, the Core HR system does not support qualifying beneficiaries due to death of employee or employee moves to Medicare. These events must be processed directly with your COBRA administrator.
COBRA Log
The COBRA log is found by navigating to System > Export Logs > COBRA Log.
The COBRA log dictates what information is sent on your COBRA files. There is a separate log for each COBRA eligible benefit.
Due to the sensitive nature of COBRA administration, please read through this article before making any changes to your COBRA log. If you have any further questions, you can contact us through our support chat. For more information, you can refer to the following article.
COBRA Log – Export Reasons
How the employees are included in the file and in which file they appear, is driven by Reason (found in the employee’s record in the COBRA log).
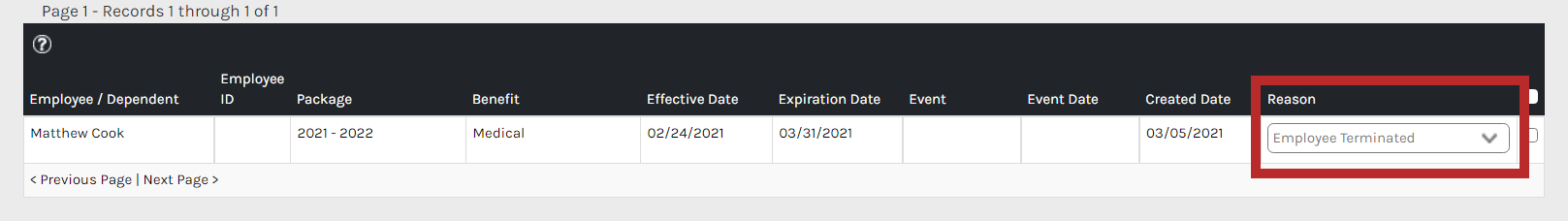
The system has 5 reasons an employee record has populated in the log.
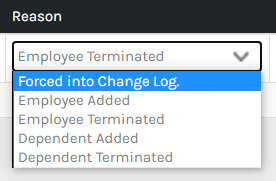
Forced into Change Log – This happens when an administrator has forced an employee’s record into the change log from the employees’ Benefits > Benefits page. This is a special case scenario wherein an employee's benefit record has to be manually placed into the change log. An example of using this log is when you need to resend a record to the COBRA vendor as a result of an update to the employee’s record in the system.
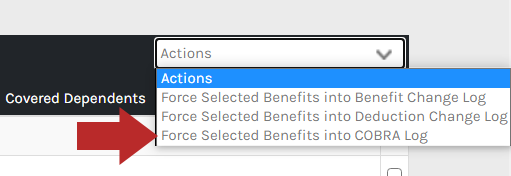
Employee Added – When an employee initially elects benefits in the system, they will be entered into the COBRA Log with a reason of "Employee Added". This will drive the record to the New Hire file.
Dependent Added – When a dependent has been added to an employee’s benefit record, the dependent will be entered into the COBRA Log. This occurs when an employee has completed a Birth event or a Marriage event. Most COBRA administrators do not require this.
Employee Terminated – When an employee has had their benefits terminated, they will be entered into the COBRA Log with a reason of "Employee Terminated".
Dependent Terminated – When a dependent has been terminated from an employee’s benefits, they will be entered into the COBRA Log with a reason of "Dependent Terminated". This will occur when an employee has been terminated through a Dependent Becomes Ineligible event (dependent becomes overage) or a Divorce or Annulment event.
Benefit Processing
Events
The most important responsibility you hold as an administrator with regard to your COBRA files, is awarding and terminating benefits correctly.
To enable employees to self-serve and declare events, you must have events configured in your system prior to terminating dependent only benefits. For additional information, you can refer to the Required Events section.
You must have termination reasons configured in your system prior to processing, awarding, and terminating employee benefits. For additional information, you can refer to the Termination Reasons section.
Events are configured within your system by navigating to Setup > Setup Properties.
From the menu bar, navigate to Employee Portal Setup > Employee Portal.
Click the Events tab
Required Events
You may click on any event to configure the event to your specifications and to activate the event. With regard to COBRA processing, you will need the following events configured and active on your employee portal at all times:
Divorce or Annulment – This event is used to process the termination of a spouse dependent from an employee’s record. When an employee successfully completes this event, the terminating spouse will send to your COBRA administrator as a qualifying beneficiary.
Marriage – This event is used to award benefits to a newly added spouse. When an employee successfully completes this event, the awarded dependent will send to your COBRA administrator as a new beneficiary.
Dependent Becomes Ineligible - This event is used to terminate an overage dependent from an employee’s record. An employee should complete this event when terminating a dependent that has recently become overage for the COBRA eligible benefit (e.g. a dependent the age of 26 is overage for a medical plan). When an employee successfully completes this event, the terminating overage dependent will send to your COBRA administrator as a qualifying beneficiary.
Administrative Updates - These events can also be assigned when terminating or awarding benefits on the administrative portal.
When processing the mid-year change for an employee’s benefits, on Step 2, you will find a dropdown of events under Reason for Change. Any of the above events may be selected during this process.
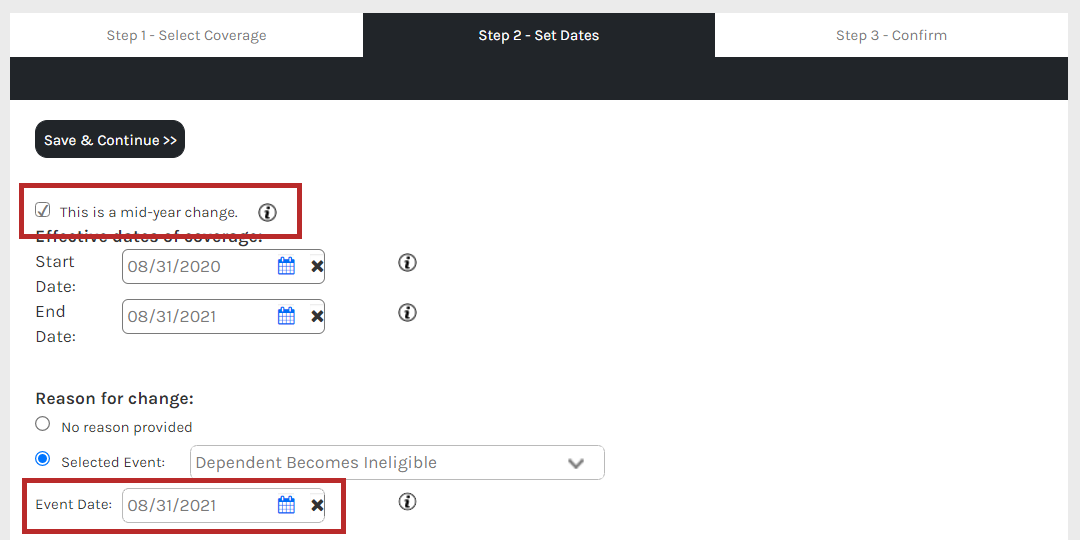
Make sure that the mid-year change is being processed the day of the event (i.e. if a dependent’s birth day is 7/17/2016, that is the event date. The Change Date is the day benefits expire plus 1. Using an overage dependent as an example, if the dependent should have coverage until the end of the month, 6/30, the Change Date should be 7/1. The Event Date is the dependent’s birthday.
If a dependent is terminating and you do not select the applicable event, they will not send on the file as a QB.
Termination Reasons
If proper termination reasons are not configured in your system prior to the implementation of your COBRA files, termination reasons will be entered in by the EDI specialist building the files.
Termination reasons can be configured by navigating to Setup > Setup Properties in the menu.

From the menu bar, navigate to Field Value Setup > Termination Reasons.
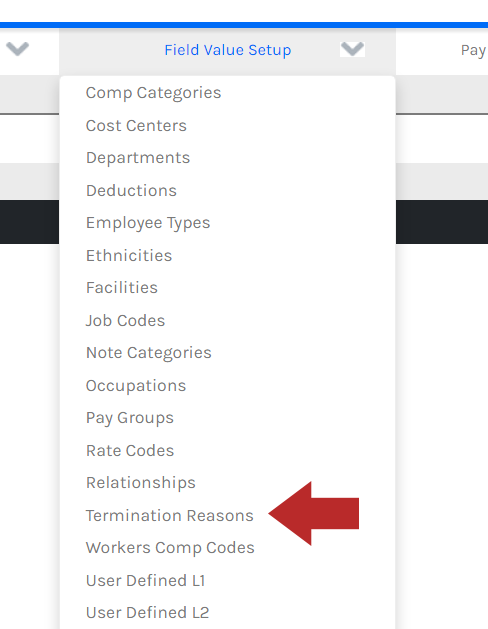
There must always be at least two termination reasons configured in your system. There will always be logic in your qualifying beneficiary file that maps against these termination reasons. One termination reason must be Reduction in Hours. This is used when you are terminating an employee that is moving from a full-time benefit eligible status to a part-time benefit ineligible status.
The second termination reason is configurable to your company’s specifications. This will be a general termination of employment reason and can be a generic “Termination” code, or can be altered and configured to your liking, such as “Voluntary Resignation”.
For assistance with setting up termination reasons, you can refer to the following article.
Terminating an Employee
When terminating an employee that has been awarded benefits, be sure to terminate the employee from the Termination Eligibility List or from the employee’s Benefits > Benefits page. From the Termination Eligibility List, you will click on the record count number to pull up the list on your screen.
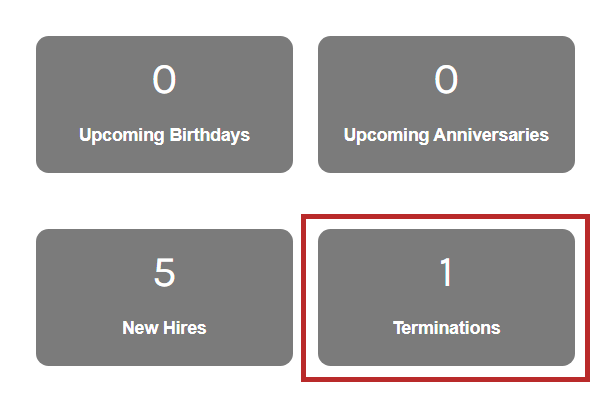
You may select the employee(s) you wish to terminate. The termination date will be prepopulated, as the employees have been terminated from their demographic screen already. Be sure to select the termination reason from the dropdown.
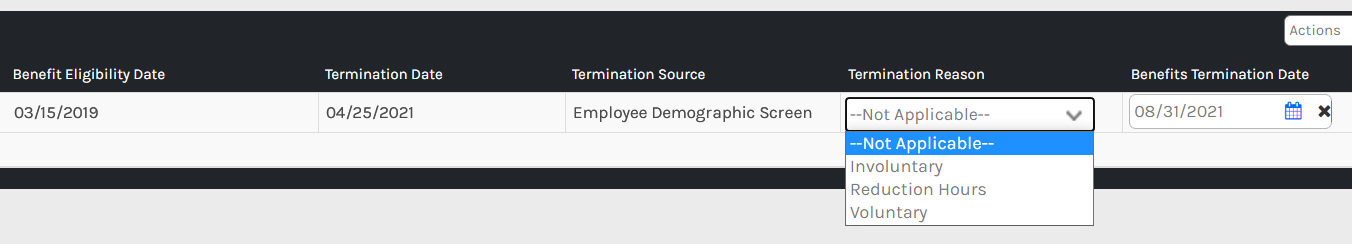
The benefits termination date can be updated, but will be pre-populated based on the termination date of the employee.
Please note that employees that change from a Full Time to a Part Time status do not populate in the Termination Eligibility List.
When terminating an employee from their Benefits > Benefits > Terminate page, you may select the employee and benefit status, termination date and reason, and the date in which the benefits terminate.
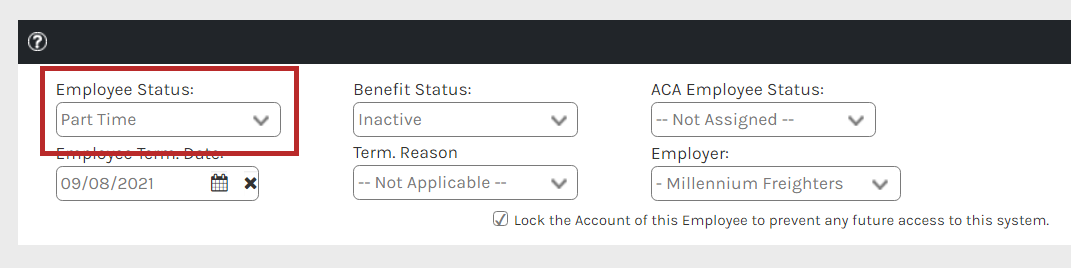
When moving an employee from Full Time to Part Time, the termination date and reason do not parse over to the demographics screen. You will need to navigate to the Employee > Employee > Demographic Info page to update the date and reason they moved to part time (reduction in hours).